by Justin Mckibben | Mar 28, 2019 | Addiction Medicine, Detox, Recovery, Sobriety
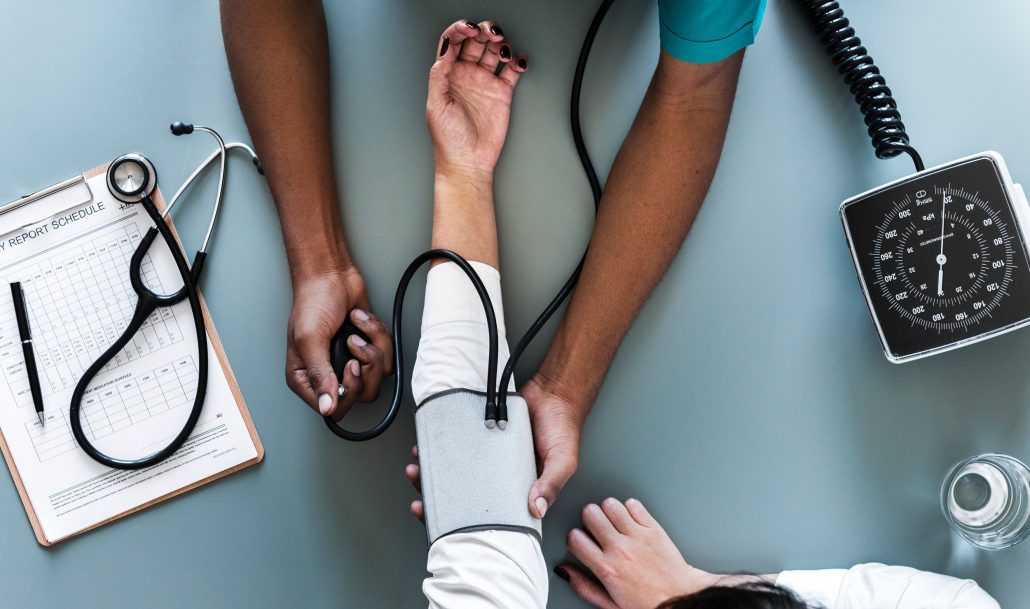
Physical Health is Important to Lasting Recovery
There is no doubt that substance use disorder has a dramatic impact on health. Physical, mental and emotional well-being always suffer when an individual becomes dangerously dependent on harmful substances. Drugs and alcohol have a variety of adverse effects on the body, ranging from painful withdrawal symptoms to lasting impairment of vital organs. Therefore, it should not come as a surprise that patients recovering from addiction often suffer from chronic health conditions.
Now, a new study published in the Journal of Addiction Medicine suggests that more than one-third of people recovering from addiction continue to suffer from a physical disease.
Studying Chronic Health Conditions in Addiction Recovery
Researchers from the Massachusetts General Hospital (MGH) Recovery Research Institute are the first to examine the national prevalence of medical conditions typically created or magnified by chronic and excessive use of drugs or alcohol. The data in the study comes from a nationally representative sample of more than 2,000 American adults. Each of these individuals described themselves as recovering from a range of substance issues, including:
Researchers then looked for the presence of diseases known to be exacerbated by drugs and alcohol, such as:
- Liver disease
- Diabetes
- Heart disease
- Tuberculosis
- HIV/AIDS
- Sexually transmitted infections (STIs)
- Cancer
- Hepatitis C
- Chronic obstructive pulmonary disease (COPD)
What they found was that out of all the adults recovering from substance abuse issues, 37% of them had been diagnosed with one or more of these nine conditions.
Additionally, researchers conclude that significant reductions in the participants’ quality of life connect to these conditions. Not to mention, researchers note that each of these health problems is known to reduce life expectancy.
Trends Relating to Different Drugs
When looking at the details of the data, there are a few trends that stand out. For instance, when compared to the general population, individuals in recovery have much higher levels of:
- Hepatitis C
- COPD
- Heart disease
- Diabetes
And in many cases, certain diseases more often correlate with certain substances. For example:
Hepatitis C
Rates of this condition were significantly higher for those recovering from opioids or stimulants than those recovering from alcohol.
HIV/AIDS and STIs
Lifetime prevalence of these health conditions was significantly higher in the group of people recovering from stimulant abuse than in the alcohol group.
Heart Disease
The lowest rates of this condition were actually found in individuals recovering from opioid addiction.
Diabetes
This health problem was discovered to be least common for those reporting cannabis as their primary substance issue
Multiple Chronic Conditions
The odds of experiencing two or more chronic physical diseases were increased by 4%- 7% due to certain factors, such as:
- Each additional substance used 10 times or more
- Older age at onset of diseases
- Resolving alcohol or drug problems later in life
Reduced Rates of Disease
Researchers also note a few elements that appear to coincide with reduced rates of physical diseases. In general, such factors include being:
There were also social stability and economic factors linked to lower rates of physical disease for those recovering from substance abuse, including:
- Having a household income greater than $50,000
- Higher education
- Being Employed
- Married or living with a partner
Some of these may be a bit of a surprise, especially considering that women are typically considered more susceptible to serious health problems associated with substance abuse.
Highlighting the Importance of Health in Recovery
According to the researchers, this study is important to a larger conversation about the quality of life for those in recovery from addiction. The lead and corresponding author David Eddie, Ph.D., research scientist at the Recovery Research Institute is an MGH clinical psychologist and an instructor in Psychology at Harvard Medical School. He states,
“We’ve known for a long time that chronic and heavy substance use can cause a multitude of diseases directly and indirectly – The extent to which these diseases and health conditions continue to persist for the millions of Americans who achieve recovery remains to be clarified, but this study highlights the fact that these negative impacts may continue to affect quality of life even when people achieve addiction recovery.”
Eddie believes it is important to appreciate that even those who overcome their issues with substance use disorder and drug dependence still face real physical diseases. In some cases, men and women who manage to finally make progress away from abusing drugs or alcohol still have to live the rest of their lives with other life-altering conditions. If the evidence points toward a better chance at young people and those with a shorter history of drug use being able to avoid chronic illness, then, of course, more effort should be put toward early intervention. Eddie adds,
“In addition, addiction treatment needs to be more seamlessly integrated with primary health care, and more research is needed to explore the complex relationships between alcohol and other drug use and physical disease.”
Moreover, this would further support the idea that we must address addiction as a public health issue. If we want to effectively address not only substance abuse but the long-term adverse effects of drugs and alcohol, we have to offer more comprehensive treatment options.
Part of building a healthy and effective foundation for recovery is a personalized treatment plan. Every individual is unique, and each person struggling with substance use disorder faces different challenges. That is why Palm Healthcare Company believes in providing customized and comprehensive care to every client. From medical detox resources to medication management and nutrition, we believe better health and well-being make lasting recovery possible. If you or someone you love is struggling, please call toll-free now. We want to help.
CALL NOW 1-888-922-5398
by Justin Mckibben | Mar 19, 2019 | Addiction Treatment, Depression, Detox, Inpatient Treatment, Mental Health, News, Outpatient Treatment
Discrimination Through Denial of Coverage

Health insurance is probably going to be one of the great debates of this period in American history. There is already plenty of contention about how to properly provide coverage for those who need it. Some claim the changes made in the last decade have gone too far. Others argue it has not gone nearly far enough. Healthcare reform is a hot button issue in our world today. Needless to say, a big part of this conversation has to do with parity coverage for mental health. Now a new landmark court ruling is going to make a monumental difference for mental health and addiction treatment insurance coverage.
Simply put, the largest behavioral health care company in America has been denying coverage to some of its most vulnerable members to save money. And now, a federal court decision may put more of a spotlight on insurance companies.
Wit v. United Behavioral Health
The case was brought in front of a federal court in Northern California against United Behavioral Health (UBH). UBH is a company that manages behavioral health services for UnitedHealthcare and other health insurers. The court found that UBH denied claims of tens of thousands of people seeking mental health and substance use disorder treatment. The company was using defective medical review criteria in order to reject claims.
In Wit v. UBH, over 50,000 individuals were reportedly denied coverage based on the flawed review criteria. 11 plaintiffs sued UBH on the behalf of these victims. One victim, in particular, is Natasha Wit. Natasha had been seeking treatment for several chronic conditions, including:
Wit was repeatedly denied coverage for her treatment, despite the fact she did have healthcare benefits that should have offered coverage. Her family ended up paying out nearly $30,000 for treatment. And they are just one of the thousands of families to face the same discrimination.
Looking at the Marks Against UBH
According to recent reports, United Behavioral Health has been failing its members in more ways than one.
Federal courts determined that UBH developed internal guidelines that were “unreasonable and an abuse of discretion” and “infected” by financial incentives designed to restrict access to care for those who should qualify for coverage. Essentially, UBH was manipulating internal guidelines to avoid providing coverage that members had every right to under the law.
For many of those struggling with substance use disorder, defective criteria for coverage can equate to a death sentence. When looking over the requirements set by UBH, it is no wonder why the courts say they are illegitimate.
Firstly, their medical-necessity criteria fail to provide coverage to those chronic and comorbid conditions. Generally accepted standards of care state these conditions should be effectively treated, even when those conditions:
- Persist
- Respond slowly to treatment
- Require extended or intensive levels of care
However, UBH set guidelines that only approve coverage for what they labeled “acute” episodes or crises. For example, only individuals who were actively suicidal or suffering from severe withdrawal could be considered for coverage.
In other words, for someone who struggled with substance use disorder or mental illness, you had to be knocking on death’s door to get a chance at treatment. The court found that these guidelines were not acceptable.
Furthermore, UBH fails to use national evidence-based guidelines for covering different levels of care for mental health and substance abuse treatment, such as:
These are guidelines that have been developed by clinical specialty nonprofit organizations.
Additionally, UBH’s guidelines improperly required reducing the level of care, even if the providers who were treating them recommended maintaining a higher level of care. So patients would be removed from more intensive residential treatment programs and pushing into some form of outpatient therapy, even if the specialists argued that they were not ready.
This is a big deal. Most recovery advocates and healthcare providers agree that insurance companies should not be the ones telling treatment providers how to care for their patients.
-
State Mandated Guidelines
Furthermore, some states have mandated specific guidelines for evaluating the medical necessity for behavioral health services. UBH was also found to have violated these requirements for reviewing substance use disorder claims as well.
The case against United Behavioral Health was filed under the Employee Retirement Income Security Act of 1974 (ERISA). This is a federal mandate that governs group health insurance policies through private employers. More specifically, ERISA requires insurance plan administrators to function in a fiduciary capacity when overseeing employee benefit plans. This includes coverage for mental health and substance use disorder treatment.
In Wit v. UBH, the court determined that UBH was in breach of its fiduciary duties by developing and employing faulty medical necessity criteria for behavioral health services. Therefore, the court alleges that UBH is in violation of its obligations under this federal law.
What Does this Mean for Addiction Treatment Insurance Coverage?
This case is exposing insurers for refusing care to people at serious risk of death by overdose or suicide. It is important to remember that UBH is not the only insurance provider trying to find ways around federal and state coverage guidelines. Given the nature of these violations, advocates believe that regulators should immediately start examining the market conduct of all healthcare plans across the country.
Judge Joseph C. Spero in Wit v. UBH also points out that the company was circumventing the Mental Health Parity and Addiction Equity Act of 2008, also known as the Federal Parity Law.
Parity law actually requires insurers to cover illnesses of the brain, such as depression or addiction, the same as illnesses of the body, such as diabetes or cancer. In his ruling on Wit v. United Behavioral Health, Judge Spero highlights an abundance of evidence that guidelines created by the UBH were designed to diminish the impact of the 2008 Parity Act in order to keep benefit costs down. In other words, it is clear that the company was actively trying to work around federal law in order to avoid providing coverage to people with mental illnesses and addictions.
For those in the mental health and addiction communities, this brings new awareness to the discriminatory practices of treating mental health conditions differently than physical conditions. The new hope is that insurance providers will understand the consequences of discrimination against those who need help. With so much going on in healthcare, the Federal Parity Law must be protected.
Far too many people suffering from mental health and substance use disorders never get the help that they need. The last thing we need in a country devastated by an opioid crisis and rising overdose death rates is to create more roadblocks to treatment resources.
Palm Healthcare Company believes that if our country is ever going to overcome the damage of the opioid epidemic, we have to offer more comprehensive treatment options to those who still suffer. Insurance companies should not be keeping people from the care they deserve. Prevention is important, but we also believe in taking care of those who are already in the grips of substance use disorder by offering compassionate and effective care. If you or someone you love is struggling, please call toll-free now. We want to help.
CALL NOW 1-888-922-5398
by Justin Mckibben | Mar 8, 2019 | Alcohol, Death, Drug Abuse, Harm Reduction, News

Two non-profit organizations recently analyzed updated data from the Center for Disease Control and Prevention (CDC) and found that deaths caused by suicide, drug overdose and alcohol rose by 6% in the year 2017, leading to an all-time high in the United States.
Record-Breaking Devastation
Altogether, drugs, alcohol, and suicide killed more than 150,000 people.
Ever since federal data collection started in 1999, the non-profit’s report claims there has never been a death rate this high attributed to these causes. A spike was observed in the national rate for deaths from alcohol, drugs, and suicide:
- Start of 2017- 9 deaths per 100,000 people
- End of 2017- 6 deaths per 100,000 people
On one hand, this is actually a slower increase than the previous two years. However, the difference was a lot over the average annual increase of 4% since 1999.
Opioid Death Rates
Probably the most obvious reasoning behind this increase would be the ongoing opioid crisis. One of the major contributing factors to the rising rates of overdose death in America is dangerous synthetic drugs making their way to the illicit market.
For one thing, deaths due to synthetic opioids like fentanyl, rose 45 % in that time. In the past five years, these deaths have actually increased tenfold. Needless to say, lawmakers and public health officials have been scrambling for years to try and solve the overdose issue in the United States.
Suicide Death Rates
Since 1999, deaths from suicide have increased by 33%. The data for 2017 indicates a significant rise in death rates:
- Start of 2017- 9 deaths per 100,000
- End of 2017- 5 deaths per 100,000
This is an increase of 4%, which is double the average annual pace over the previous decade. More specifically, from 2008 to 2017:
- Suicide by suffocation increased by 42%
- Suicide by firearm increased by 22%
The highest suicide rates are typically in rural areas, including:
- West Virginia
- New Mexico
- Ohio
- Alaska
- New Hampshire
One thing to point out is that some researchers believe that suicides are actually under-reported. This may be in part due to the stigma surrounding mental disorders, but also largely due to mislabeling the cause of death. For instance, some cases may be recorded as overdoses or accidents that are actually intentional.
Alcohol Death Rates
As far as alcohol-related death rates are concerned, some suspect that higher proof alcohols becoming increasingly popular in the last decade has also contributed to health issues and deaths. In fact, between 2002 and 2013:
- The amount of how much alcohol Americans consumed only increased by 6%.
- Estimates to determine how much alcohol is typically drunk have remained the same.
- Health problems as a result of drinking spiked in the same time frame.
Meanwhile, some drinks have a dramatically higher alcohol-by-volume (ABV) percentage. Between 2002 and 2016, the average alcohol by volume grew across the board:
- Beer ABV increased an average of 2%
- Wine ABV increased an average of 6%
- Liquor ABV increased an average of 4%
According to another analysis by the Institute for Health Metrics and Evaluation at the University of Washington, from 2007 to 2017:
- The number of deaths attributable to alcohol increased by 35%
- Deaths among women rose 85%
- Deaths among men rose 29%
One positive piece of data is that the study suggests teen drinking deaths actually decreased by 16%. Still, alcohol has contributed plenty to the rising death rates.
Addressing Underlying Issues
With the highest death rates due to drugs, alcohol, and suicide in recorded history, it goes without saying that a lot more needs to be done to promote treatment resources and prevention. With the failed War on Drugs has taught us what is not working, many have turned to strategies that focus on the preservation of life more than punishing those struggling with addiction. Harm reduction efforts like naloxone expansion and needle exchange programs have made some real progress. Some have even begun exploring the possibility of establishing safe injection sites.
Additionally, there needs to be more put into comprehensive treatment. Most experts agree there is a need for broader efforts to address the underlying causes of alcohol and drug use, and suicide. Having access to effective mental health care and addiction treatment resources can significantly impact the well-being of those most at risk. Long-term recovery offers those most likely to die as a result of drug use or suicide a way out.
This would also include more funding and support for programs that reduce risk factors. A major aspect of prevention when it comes to substance abuse and mental health has to do with trauma and adverse childhood experiences. Research has suggested there is a notable connection between the risk of drug and alcohol abuse and suicide and childhood trauma.
There were five states where death rates due to drugs, alcohol, and suicide decreased:
- Massachusetts
- Oklahoma
- Rhode Island
- Utah
- Wyoming
Hopefully, as new initiatives push forward to save lives and offer prevention, we will see more states with decreasing death rates. Overall, we can hope that better opportunities for treatment and support will lead to an improvement in public health. Meanwhile, raising awareness and education are crucial to turning this trend around.
With their highest death rates in history, substance abuse and suicide are some of the most important public health issues facing Americans today. If you or someone you love is struggling, please call toll-free now.
CALL NOW 1-888-922-5398




